Address
Opp. Khalsa College for Boys, near BSF Chowk, Jalandhar
Call
+91 98140 61069
Opp. Khalsa College for Boys, near BSF Chowk, Jalandhar
+91 98140 61069

Infertility affects up to 15% of couples, and in nearly half of these cases, a male factor is involved. At Sarvodya Hospital, under Dr. Rajesh Aggarwal, we understand how emotionally challenging infertility can be — and we’re here to help. As a fellowship-trained urologist specializing in male reproductive health, Dr. Rajesh Aggarwal offers advanced diagnostics and effective treatment options for male infertility.
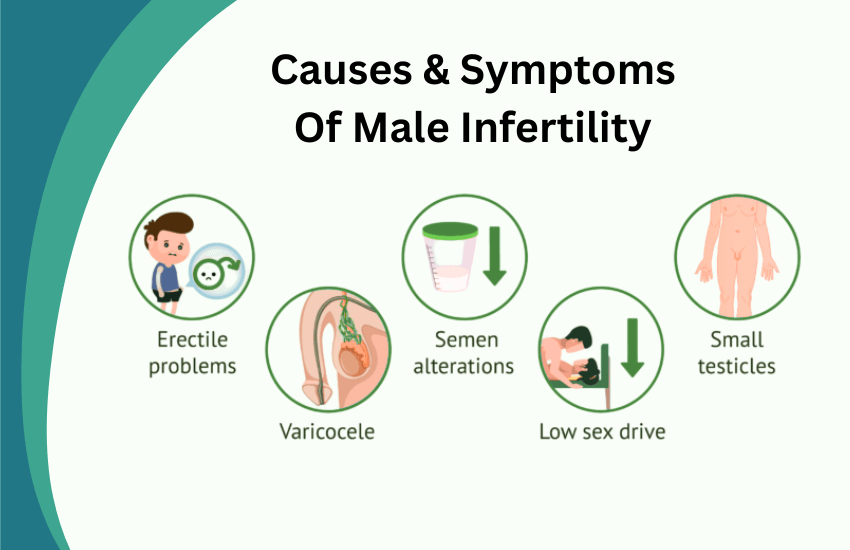
Male infertility refers to a man’s inability to cause pregnancy in a fertile female partner after 12 months of regular, unprotected intercourse. It can stem from issues with sperm production, sperm function, or sperm delivery.
Common Causes of Male Infertility
There are many potential causes of male infertility, including:
Often, male infertility has no obvious symptoms aside from the inability to conceive. However, some men may experience:
At your consultation, we take a thorough medical and reproductive history, followed by a physical exam and appropriate testing, which may include:
Our approach is comprehensive and confidential, with a focus on identifying the root cause of infertility.
Treatment depends on the underlying cause and may include: